Keratoconus
Early Diagnosis, Treatment, and Protecting Your Vision
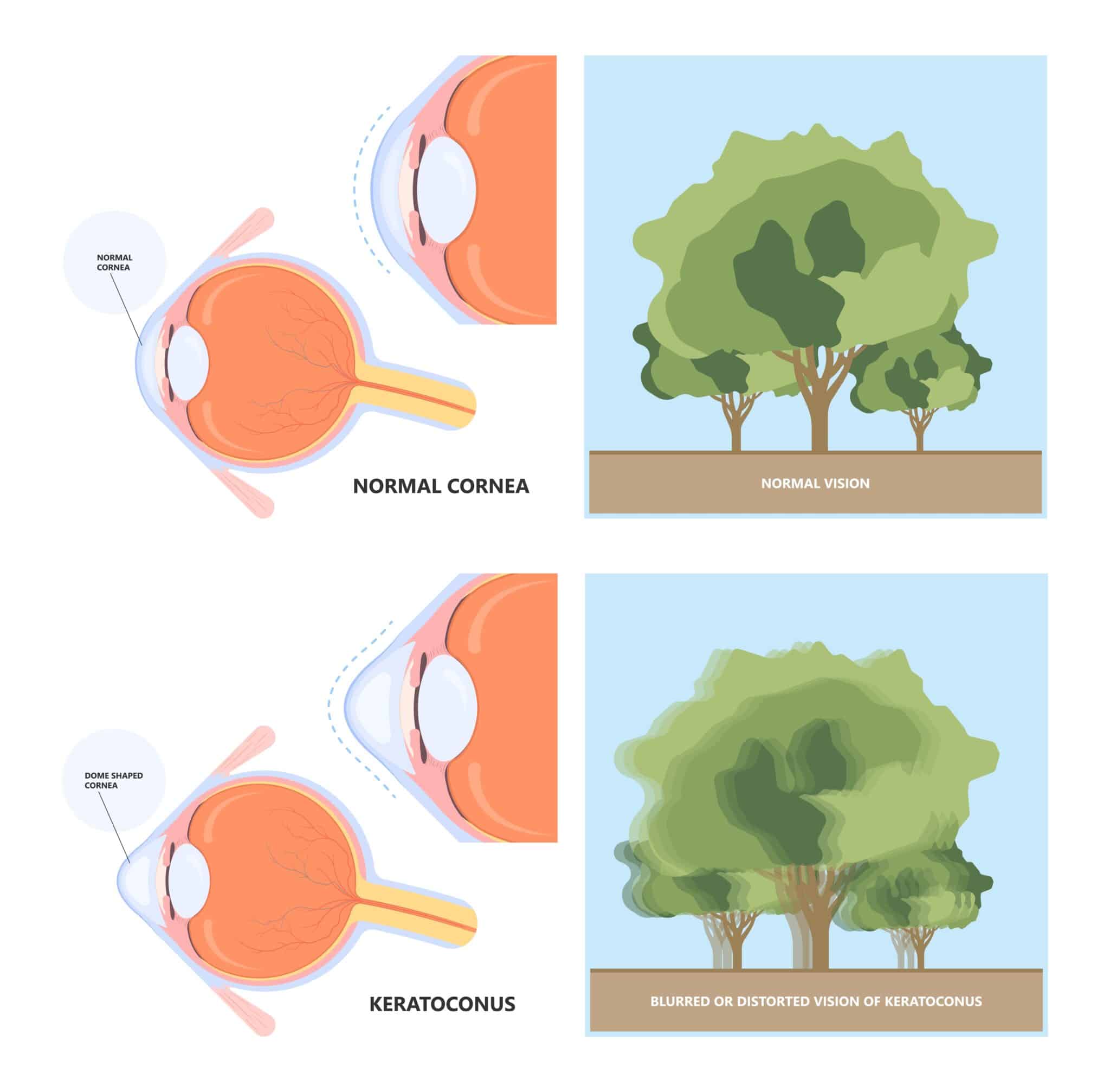
Keratoconus is a progressive eye condition that affects the cornea — the clear, dome-shaped front surface of the eye responsible for focusing light. In keratoconus, the normally round cornea gradually thins and begins to bulge forward into a cone-like shape. This irregular shape prevents light from focusing properly on the retina, leading to distorted and blurred vision.
Keratoconus often begins in the teenage years or early adulthood and may worsen over time if not properly diagnosed and treated. Early detection is critical, as modern treatments can stop progression and preserve vision.


What Causes Keratoconus?
Keratoconus is considered a multifactorial condition with both genetic and environmental influences. It is commonly inherited, meaning it can run in families. If one family member is diagnosed, it is important that siblings and children undergo screening examinations, even if they have no symptoms. Early corneal imaging can detect subtle signs of the condition before vision becomes noticeably affected.
Another major contributing factor is chronic eye rubbing. Repeated mechanical trauma from eye rubbing can weaken the corneal structure and accelerate progression of the disease. Patients diagnosed with keratoconus must strictly avoid rubbing their eyes. Managing allergies and dry eye, which often trigger rubbing, is an essential part of treatment.
Symptoms of Keratoconus
As the cornea becomes more irregular, patients may experience:
In early stages, glasses or soft contact lenses may provide adequate correction. However, as the cornea becomes more irregular, standard lenses often fail to provide clear vision.

Advanced Diagnosstic Techniques
Early diagnosis of keratoconus is essential. Modern technology allows us to detect even subtle changes in corneal shape and thickness before significant vision loss occurs.
Diagnostic tools include:
These imaging techniques are painless, quick, and critical for early detection. Because keratoconus can progress silently before noticeable symptoms develop, routine screening is especially important for patients with a family history.
The Importance of Early Diagnosis
One of the most important aspects of managing keratoconus is understanding that modern treatment can stop progression — but it cannot reverse damage that has already occurred.
If the cornea has already become significantly distorted, vision loss may be permanent. While vision can often be improved with specialty contact lenses, the structural changes to the cornea cannot be undone. For this reason, early diagnosis and timely treatment are crucial.
Treatment: Two Essential Components
Treatment of keratoconus involves two distinct goals:
- Stopping progression of the disease
- Correcting vision loss
1. Corneal Crosslinking (Stopping Progression)
Corneal crosslinking is the only treatment proven to halt the progression of keratoconus. This office-based procedure strengthens the cornea by increasing the natural bonds (crosslinks) between collagen fibers within the corneal tissue.
The procedure involves applying riboflavin (vitamin B2) drops to the cornea, followed by controlled ultraviolet (UV) light exposure. This combination strengthens the corneal structure and stabilizes it.
There are two primary approaches:
Your surgeon will determine which technique is most appropriate based on your specific corneal measurements.
Crosslinking is performed in the office and generally takes about an hour. A soft bandage contact lens is placed on the eye at the end of the procedure to promote healing and comfort. The bandage lens typically remains in place for approximately five days.
Most patients recover quickly and resume normal activities shortly thereafter. While mild discomfort and light sensitivity may occur during the first few days, healing progresses rapidly.
Importantly, crosslinking usually needs to be performed only once. It is very rare for the procedure to need to be repeated.

2. Vision Correction (Rigid or Scleral Contact Lenses)
While crosslinking stops progression, it does not reverse the irregular shape that has already developed. Therefore, many patients require specialty contact lenses to achieve clear vision.
Rigid gas-permeable (hard) lenses and scleral lenses are commonly used. These lenses create a smooth optical surface over the irregular cornea, dramatically improving clarity. Scleral lenses, which rest on the white part of the eye rather than the cornea itself, are often particularly comfortable and effective.
Together, crosslinking and specialty lenses provide both structural stability and visual rehabilitation.
Protecting Your Vision for the Future
Keratoconus is a manageable condition when diagnosed early. Avoiding eye rubbing, treating allergies promptly, and screening family members are critical preventive steps.
With early detection and timely crosslinking, progression can be halted, preserving the cornea and preventing severe vision loss. Combined with modern specialty contact lenses, most patients can maintain excellent functional vision and avoid more invasive procedures such as corneal transplantation.
If you or a family member have experienced frequent prescription changes, increasing astigmatism, or blurred vision that cannot be fully corrected with glasses, a comprehensive corneal evaluation is recommended.
